Pacemaker Codes
No discussion of pacemakers can take place without an understanding
of the generic pacemaker code, which has been published by the North American Society
of Pacing and Electrophysiology (NASPE) and British Pacing and Electrophysiology
Group (BPEG). This code (NBG
†
was
*Although many authors and
references identify this device as an "automatic implantable cardioverter-defibrillator
or AICD," the term "AICD" is a brand name and belongs to Cardiac Pacemakers Inc (CPI),
which has been acquired by Guidant Medical Corporation, St. Paul, MN. The term "PCD"
(for "Programmable Cardioverter-Defibrillator") belongs to the Medtronic Corporation.
†The NBG
code is a joint project from NASPE (the "N") and BPEG (the "B"). The "G" stands
for generic.
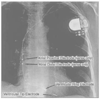 Figure 35-1
Pacemaker with one quadripolar lead that provides atrial
and ventricular sensing and ventricular pacing. This chest x-ray film shows a number
of features of a modern pacing system. The generator is located in the left pectoral
region. The single lead enters the subclavian vein under the clavicle but superficial
to the first rib (a common site for lead problems, although no problem is demonstrated
here). In this device, there are two electrodes in the right atrium that can provide
sensing to detect intrinsic atrial activity. The ventricular portion of the lead
shows the classic bipolar pattern, with a ring electrode just proximal to the tip
electrode, and these electrodes can be used for sensing intrinsic ventricular activity
and for depolarizing the ventricle. This is a ventricular pacing system with pacing
in the triggered and inhibited mode (VDD), and this configuration is placed into
patients with a functioning sinus node but a nonfunctioning atrioventricular node.
This system cannot be used to depolarize the atrium. Because the surface electrocardiogram
often demonstrates ventricular pacing that tracks the atrial activity, inspection
of the surface electrocardiogram typically produces an erroneous diagnosis of a dual
chamber (DDD) pacemaker.
Figure 35-1
Pacemaker with one quadripolar lead that provides atrial
and ventricular sensing and ventricular pacing. This chest x-ray film shows a number
of features of a modern pacing system. The generator is located in the left pectoral
region. The single lead enters the subclavian vein under the clavicle but superficial
to the first rib (a common site for lead problems, although no problem is demonstrated
here). In this device, there are two electrodes in the right atrium that can provide
sensing to detect intrinsic atrial activity. The ventricular portion of the lead
shows the classic bipolar pattern, with a ring electrode just proximal to the tip
electrode, and these electrodes can be used for sensing intrinsic ventricular activity
and for depolarizing the ventricle. This is a ventricular pacing system with pacing
in the triggered and inhibited mode (VDD), and this configuration is placed into
patients with a functioning sinus node but a nonfunctioning atrioventricular node.
This system cannot be used to depolarize the atrium. Because the surface electrocardiogram
often demonstrates ventricular pacing that tracks the atrial activity, inspection
of the surface electrocardiogram typically produces an erroneous diagnosis of a dual
chamber (DDD) pacemaker.
TABLE 35-1 -- NASPE/BPEG revised (2002) NBG pacemaker code
*
|
Position I |
Position II |
Position III |
Position IV |
Position V |
|
(Chamber Paced) |
(Chamber Sensed) |
(Response to Sensed Event) |
(Programmability, Rate Modulation) |
(Multisite Pacing) |
|
O = none |
O = none |
O = none |
O = none |
O = none |
|
A = atrium |
A = atrium |
I = inhibited |
R = rate modulation |
A = atrium |
|
V = ventricle |
V = ventricle |
T = triggered |
|
V = ventricle |
|
D = dual (A + V) |
D = dual (A + V) |
D = dual (T + I) |
|
D = dual (A + V) |
|
NBG: North American Society of Pacing and Electrophysiology
(N) and British Pacing and Electrophysiology Group (B) generic (G) pacemaker code. |
*The
generic pacemaker code,[8]
initially published in
1983, was last revised in 2002 in an effort to keep current with technologic developments
in the pacing field. The NBG code is a joint project of the North American Society
of Pacing and Electrophysiology (NASPE) and the British Pacing and Electrophysiology
Group (BPEG).
initially published in 1983 and was last revised in 2002.[8]
It describes the basic behavior of the pacing device ( Table
35-1
). Pacemakers also come with a variety of terms generally unfamiliar
to the anesthesiologist, many of which are shown in the glossary at the end of this
chapter.
The first two positions of this code (i.e., chamber paced and
chamber sensed) seem relatively straightforward. Although early pacemakers provided
only ventricular support, current models can provide pacing in the atria and ventricles,
and these devices can also be programmed to determine intrinsic activity in these
chambers as well. The code does not describe the array of diagnostic data that can
be accumulated by these devices.
Probably the most confusing aspect of the NBG code is the third
position (i.e., response to sensed event). Most pacemakers are programmed either
to the DDD (dual chamber pacing and sensing, both triggered and inhibited mode) or
VVI mode (for single chamber, ventricular pacing in the inhibited mode). Two other
modes frequently found are VDD (ventricular pacing with atrial tracking) and DDI
(dual chamber pacing and sensing, but inhibited mode only). In the United States,
it is uncommon to find an atrial-only pacemaker (AAI), but these devices are indeed
implanted in patients with sinus node disease in other countries. The third position
describes the following behavior:
- D (dual): For DDD pacemakers, atrial pacing will take place in the "inhibited"
mode; i.e., the pacing device will emit an atrial pulse if no sensed atrial event
(or intervening ventricular event, since any ventricular event will reset atrial
timing) takes place within the appropriate timeframe. In DDD or VDD devices, once
an atrial event has occurred (whether native or paced), the pacing device will ensure
that a ventricular event follows (up to the Upper Tracking Rate [see glossary]).
Dual response pacemakers are used to provide atrioventricular (AV) synchrony.
- I (inhibited): The pacer will emit a pulse to the appropriate chamber
unless it detects intrinsic electrical activity. In DDI mode, AV synchrony is provided
only when the pacemaker paces the atrial chamber. If intrinsic atrial activity is
present, then no AV synchrony is provided by the pacemaker.
- T (triggered): The pacing device will emit a pulse only in response to
a sensed event. Triggered mode is used when the device is being tested.
The VDD and DDI modes deserve further comment. VDD pacing is
used for the patient with AV nodal dysfunction but intact and appropriate sinus node
behavior. VDD pacing is accomplished with a single lead that incorporates atrial
sensing electrodes and ventricular conductors that can pace and sense (see Fig.
35-1
). A VDD device has no atrial pacing capability. As a result, in
a patient who depends on atrial contraction to augment cardiac output, events that
produce VVI pacing (e.g., sinus rate below the programmed rate, battery depletion)
or asynchronous ventricular pacing (e.g., magnet placement in many devices, electromagnetic
interference) can lead to deteriorating hemodynamics.[9]
[10]
DDI is rarely used as a primary mode of pacing. DDI pacing is
indicated for the patient who has a dual-chamber pacemaker and has episodes of paroxysmal
atrial dysrhythmia (e.g., paroxysmal atrial fibrillation). DDI pacing prevents high
ventricular rates (i.e.; pacing at the upper tracking rate) that could result from
attempted tracking of the atrial arrhythmia, and it provides AV synchrony only when
the atrium is paced. Some DDD pacemakers are programmed to enter the DDI mode on
the detection of high (programmable) atrial rates (called Mode Switch, Automatic
Mode Switch, or Atrial Tachy Response, depending on manufacturer). For the DDD pacemaker
that has switched to DDI, perturbations (e.g., such as atrial rates greater than
400/min), electromagnetic interference from the ESU or magnet placement and removal)
can cause the pacemaker to transiently revert back to the DDD mode, with resultant
appearance of AV pacing or ventricular pacing at the upper tracking rate (see "Pacemaker
Magnets").
Rate modulation (the fourth position) also remains a poorly understood
concept. Because some patients cannot increase their heart rate in response to increased
oxygen demand (chronotropic incompetence), pacemaker manufacturers have devised a
number of mechanisms to detect "patient exercise," such as sensors that detect vibration,
respiration, and pressure ( Table 35-2
).
As the sensor detects "exercise," it increases the pacing rate (termed "sensor indicated
rate"). As the exercise tapers, this sensor indicated rate returns to the programmed
LRL. The sensitivity of these sensors to their exercise signals and the rates of
change in pacing are programmable features in current generators.
With the 2002 revision of the NBG, the fifth column now describes
multisite pacing functionality (it had been used to describe antitachycardia function,
but this scheme has been abandoned and a generic defibrillator code has been established).
Atrial multisite pacing is being investigated as a means to prevent atrial fibrillation,
[11]
and ventricular multisite pacing is an acceptable
treatment for pacing the patient with a dilated cardiomyopathy.[12]
[13]
[14]
 Figure 35-1
Pacemaker with one quadripolar lead that provides atrial
and ventricular sensing and ventricular pacing. This chest x-ray film shows a number
of features of a modern pacing system. The generator is located in the left pectoral
region. The single lead enters the subclavian vein under the clavicle but superficial
to the first rib (a common site for lead problems, although no problem is demonstrated
here). In this device, there are two electrodes in the right atrium that can provide
sensing to detect intrinsic atrial activity. The ventricular portion of the lead
shows the classic bipolar pattern, with a ring electrode just proximal to the tip
electrode, and these electrodes can be used for sensing intrinsic ventricular activity
and for depolarizing the ventricle. This is a ventricular pacing system with pacing
in the triggered and inhibited mode (VDD), and this configuration is placed into
patients with a functioning sinus node but a nonfunctioning atrioventricular node.
This system cannot be used to depolarize the atrium. Because the surface electrocardiogram
often demonstrates ventricular pacing that tracks the atrial activity, inspection
of the surface electrocardiogram typically produces an erroneous diagnosis of a dual
chamber (DDD) pacemaker.
Figure 35-1
Pacemaker with one quadripolar lead that provides atrial
and ventricular sensing and ventricular pacing. This chest x-ray film shows a number
of features of a modern pacing system. The generator is located in the left pectoral
region. The single lead enters the subclavian vein under the clavicle but superficial
to the first rib (a common site for lead problems, although no problem is demonstrated
here). In this device, there are two electrodes in the right atrium that can provide
sensing to detect intrinsic atrial activity. The ventricular portion of the lead
shows the classic bipolar pattern, with a ring electrode just proximal to the tip
electrode, and these electrodes can be used for sensing intrinsic ventricular activity
and for depolarizing the ventricle. This is a ventricular pacing system with pacing
in the triggered and inhibited mode (VDD), and this configuration is placed into
patients with a functioning sinus node but a nonfunctioning atrioventricular node.
This system cannot be used to depolarize the atrium. Because the surface electrocardiogram
often demonstrates ventricular pacing that tracks the atrial activity, inspection
of the surface electrocardiogram typically produces an erroneous diagnosis of a dual
chamber (DDD) pacemaker.