ACUTE NORMOVOLEMIC HEMODILUTION
ANH is the removal of whole blood from a patient, while restoring
the circulating blood volume with an acellular fluid shortly before an anticipated
significant surgical blood loss. To minimize the manual labor associated with hemodilution,
the blood should be collected in standard blood bags containing anticoagulant on
a tilt-rocker with automatic cutoff via volume sensors. The blood is then stored
at room temperature and reinfused during surgery after major blood loss has ceased,
or sooner if indicated. Simultaneous infusions of crystalloid (3 mL crystalloid
for each 1 mL of blood withdrawn) and colloid (dextrans, starches, gelatin, albumin
[1 mL for each 1 mL of blood withdrawn]) have been recommended.[50]
Blood units are reinfused in the reverse order of collection since the first unit
collected; therefore the last unit transfused, has the highest hematocrit and concentration
of coagulation factors and platelets. While this technique has been primarily developed
and utilized in Europe, increasing interest in the United States has led to data
[51]
that show promise in the use of ANH as an alternative
method of autologous blood procurement. Augmented hemodilution (replacement of ANH
collected in part by synthetic oxygen carriers) is an integral part of many Phase
III studies designed to obtain FDA approval for artificial oxygen carriers.
Physiologic Considerations
Conserved Red Blood Cell Mass
The chief benefit of ANH is the reduction of RBC losses when whole
blood is shed perioperatively at lower hematocrit levels after ANH is completed.
[52]
Mathematical modeling has suggested that severe
ANH to preoperative hematocrit levels of less than 20%, accompanied by substantial
blood losses, would be required before the red
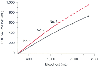 Figure 48-1
The relationship between whole blood volume (mL) lost
(abscissa) and red blood cell (RBC) volume lost (ordinate) in a 100-kg patient undergoing
hemodilution. RBC volume lost with 2800 mL whole blood lost intraoperatively after
hemodilution of 1500 mL whole blood (○-○). RBC volume lost with 2800 mL
whole blood lost during hemodilution at each of three 500 mL volumes (—).
Cumulative RBC volume lost intraoperatively, derived for 2800 mL whole blood lost
if hemodilution had not been performed (- - -). A net of 215 mL reduction in RBC
volume lost with hemodilution is illustrated by the divergence of the two curves.
(From Goodnough LT, Grishaber JE, Monk TG, et al: Acute normovolemic hemodilution
in patients undergoing radical suprapubic prostatectomy: A case study analysis.
Anesth Analg 78:932–937, 1994, with permission.)
Figure 48-1
The relationship between whole blood volume (mL) lost
(abscissa) and red blood cell (RBC) volume lost (ordinate) in a 100-kg patient undergoing
hemodilution. RBC volume lost with 2800 mL whole blood lost intraoperatively after
hemodilution of 1500 mL whole blood (○-○). RBC volume lost with 2800 mL
whole blood lost during hemodilution at each of three 500 mL volumes (—).
Cumulative RBC volume lost intraoperatively, derived for 2800 mL whole blood lost
if hemodilution had not been performed (- - -). A net of 215 mL reduction in RBC
volume lost with hemodilution is illustrated by the divergence of the two curves.
(From Goodnough LT, Grishaber JE, Monk TG, et al: Acute normovolemic hemodilution
in patients undergoing radical suprapubic prostatectomy: A case study analysis.
Anesth Analg 78:932–937, 1994, with permission.)
cell volume "saved" by ANH would become clinically important.[53]
A clinical analysis of patients who had undergone "minimal" ANH (representing 15%
or less of patients' blood volume) estimated that only 100 mL of RBCs (the equivalent
of 1/2 unit of blood) was "saved" under these conditions.[55]
With moderate hemodilution, (target hematocrit levels of 28%), the "savings" becomes
more substantial. The removal of three blood units in a patient who subsequently
underwent a blood loss of 2600 mL resulted in surgical RBC losses "saved" by hemodilution
of 215 mL, or the equivalent of 1 allogeneic blood unit[54]
( Fig. 48-1
). This RBC volume
approaches the RBC volume expansion generated by autologous blood predonation under
standard phlebotomy conditions.
The benefit of ANH as determined in a mathematical model[50]
is illustrated in Figure 48-2
.
An adult with an estimated 5-Liter blood volume and an initial hematocrit of 40%,
with surgical blood losses of up to 3000 mL would result in a hematocrit level that
would remain 25% postoperatively without an autologous blood intervention. This
level is generally considered safe for patients without known risk factors. In this
model, the performance of ANH with initial hematocrit levels of 40% to 45% would
allow up to 2500 to 3500 mL surgical blood loss; yet the nadir level of hematocrit
could be maintained at 28%.
Improved Oxygenation
Withdrawal of whole blood and replacement with crystalloid or
colloid solution decreases arterial oxygen content, but compensatory hemodynamic
mechanisms and the existence of surplus oxygen-delivery capacity make ANH safe.
A sudden decrease in RBC concentration lowers
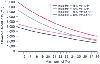 Figure 48-2
The maximum allowable blood loss in a patient with a
blood volume of 5,000 mL and an initial hematocrit level of 45% (the red lines) or
40% (the black and gray lines), with and without acute normovolemic hemodilution
(ANH). (From Goodnough LT, Brecher ME, Monk TG: Acute normovolemic hemodilution
in surgery. Hematology 2:413–420, 1992, with permission.)
Figure 48-2
The maximum allowable blood loss in a patient with a
blood volume of 5,000 mL and an initial hematocrit level of 45% (the red lines) or
40% (the black and gray lines), with and without acute normovolemic hemodilution
(ANH). (From Goodnough LT, Brecher ME, Monk TG: Acute normovolemic hemodilution
in surgery. Hematology 2:413–420, 1992, with permission.)
blood viscosity, thereby decreasing peripheral resistance and increasing cardiac
output. If cardiac output can effectively compensate, oxygen delivery to the tissues
at a hematocrit of 25% to 30% is as good as, but no better than, oxygen delivery
at a hematocrit of 30% to 35%.[56]
Preservation of Hemostasis
Because blood collected by ANH is stored at room temperature and
is usually returned to the patient within 8 hours of collection, there is little
deterioration of platelets or coagulation factors. The hemostatic value of blood
collected by ANH is of questionable benefit for orthopedic or urologic surgery because
plasma and platelets are rarely indicated in this setting. Its value in protecting
plasma and platelets from the acquired coagulopathy of extracorporeal circulation
in cardiac surgery (known as "blood pooling") is better established.[57]
 Figure 48-1
The relationship between whole blood volume (mL) lost
(abscissa) and red blood cell (RBC) volume lost (ordinate) in a 100-kg patient undergoing
hemodilution. RBC volume lost with 2800 mL whole blood lost intraoperatively after
hemodilution of 1500 mL whole blood (○-○). RBC volume lost with 2800 mL
whole blood lost during hemodilution at each of three 500 mL volumes (—).
Cumulative RBC volume lost intraoperatively, derived for 2800 mL whole blood lost
if hemodilution had not been performed (- - -). A net of 215 mL reduction in RBC
volume lost with hemodilution is illustrated by the divergence of the two curves.
(From Goodnough LT, Grishaber JE, Monk TG, et al: Acute normovolemic hemodilution
in patients undergoing radical suprapubic prostatectomy: A case study analysis.
Anesth Analg 78:932–937, 1994, with permission.)
Figure 48-1
The relationship between whole blood volume (mL) lost
(abscissa) and red blood cell (RBC) volume lost (ordinate) in a 100-kg patient undergoing
hemodilution. RBC volume lost with 2800 mL whole blood lost intraoperatively after
hemodilution of 1500 mL whole blood (○-○). RBC volume lost with 2800 mL
whole blood lost during hemodilution at each of three 500 mL volumes (—).
Cumulative RBC volume lost intraoperatively, derived for 2800 mL whole blood lost
if hemodilution had not been performed (- - -). A net of 215 mL reduction in RBC
volume lost with hemodilution is illustrated by the divergence of the two curves.
(From Goodnough LT, Grishaber JE, Monk TG, et al: Acute normovolemic hemodilution
in patients undergoing radical suprapubic prostatectomy: A case study analysis.
Anesth Analg 78:932–937, 1994, with permission.) Figure 48-2
The maximum allowable blood loss in a patient with a
blood volume of 5,000 mL and an initial hematocrit level of 45% (the red lines) or
40% (the black and gray lines), with and without acute normovolemic hemodilution
(ANH). (From Goodnough LT, Brecher ME, Monk TG: Acute normovolemic hemodilution
in surgery. Hematology 2:413–420, 1992, with permission.)
Figure 48-2
The maximum allowable blood loss in a patient with a
blood volume of 5,000 mL and an initial hematocrit level of 45% (the red lines) or
40% (the black and gray lines), with and without acute normovolemic hemodilution
(ANH). (From Goodnough LT, Brecher ME, Monk TG: Acute normovolemic hemodilution
in surgery. Hematology 2:413–420, 1992, with permission.)